This content is provided for informational purposes only and does not constitute medical advice. Consult a qualified orthopedic surgeon or healthcare professional for any decisions concerning your health and treatment options.
Localized knee arthritis confined to a single compartment presents a clinical opportunity that many patients overlook: the chance to preserve healthy joint structures whilst addressing pain at its source. Unlike total knee replacement, which resurfaces the entire joint, partial knee replacement—technically termed unicompartmental knee arthroplasty—targets only the damaged medial or lateral compartment, leaving intact ligaments, cartilage, and bone undisturbed. This selective approach translates into smaller incisions, reduced tissue trauma, and a recovery trajectory measured in weeks rather than months. Yet success hinges entirely on one critical factor: rigorous patient selection. Registry data and clinical guidelines converge on a single truth—when arthritis remains isolated and ligament integrity is preserved, partial replacement delivers exceptional outcomes. When those criteria are compromised, the procedure falters. Understanding whether you meet these exacting standards determines not just surgical success, but your long-term mobility, pain relief, and quality of life for the next two decades.
Critical facts before your consultation:
- Candidacy requires arthritis isolated to one compartment with stable anterior and posterior cruciate ligaments—multi-compartmental disease disqualifies you
- Robotic-assisted systems enhance implant alignment precision, reducing the risk of early loosening and optimising long-term durability
- Independent walking typically resumes within 2-3 weeks; complete rehabilitation spans 3-6 months, significantly faster than total replacement timelines
- Implants last 10-20 years in appropriately selected patients, with registry data showing year-on-year reductions in revision surgery when strict selection criteria are met
- Surgeon volume matters—NHS commissioning policies require a minimum of 12 unicompartmental procedures annually to maintain technical proficiency
Are You a Suitable Candidate? The Clinical Selection Criteria
The central misconception surrounding partial knee replacement is that any degree of knee arthritis qualifies you for the procedure. Clinical reality paints a far more exacting picture. Statement 2 of NICE quality standard QS206 stipulates that adults with isolated medial compartmental osteoarthritis must be offered the choice between partial and total replacement—but only when both clinical and radiological assessment confirm both options are suitable. That conditional clause is where many candidacies collapse.
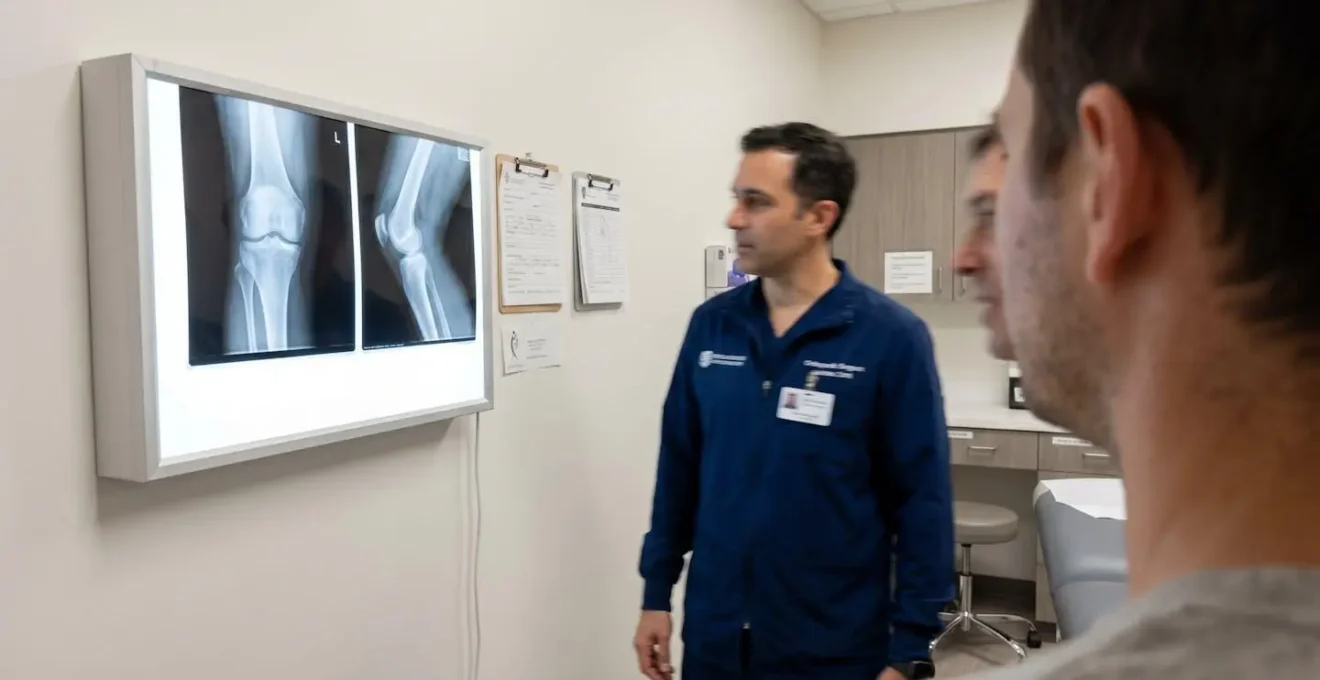
Ideal candidates share a specific clinical profile: arthritis confined to one knee compartment (typically the medial, or inner, weight-bearing surface), intact cruciate ligaments (ACL and PCL), and a knee that retains full or near-full range of motion despite pain. Imagine a patient who experiences sharp medial knee pain when kneeling in the garden or descending stairs, yet whose X-rays reveal pristine lateral and patellofemoral compartments. That patient represents the surgical sweet spot. Conversely, if imaging shows cartilage degradation across multiple compartments, or if ligament tears compromise joint stability, partial replacement becomes inappropriate—no matter how appealing the shorter recovery sounds.
Why patient selection determines success: Clinical evidence suggests that the most common reason for suboptimal outcomes is inappropriate patient selection. When partial replacement is performed despite arthritis having progressed beyond a single compartment, implant survival rates drop markedly. Clinical evidence suggests revision surgery rates increase by approximately 40-50% when strict candidacy criteria are ignored, according to registry outcome analyses. The procedure itself does not fail—the patient selection process fails.
These evidence-based selection failures underscore why self-assessment, whilst useful for preliminary orientation, cannot substitute for specialist imaging and clinical examination. The following decision framework helps identify whether your symptoms align with candidacy criteria, but definitive evaluation requires consultant orthopaedic assessment.
- Is your knee pain confined to one side (inner or outer) rather than across the entire joint?
If pain radiates across the entire front and sides of your knee, multi-compartmental arthritis is likely. Partial replacement requires isolated pain corresponding to a single compartment.
- Does your knee feel stable when walking, without a sensation of giving way or buckling?
Intact ligaments are mandatory. If your knee feels unstable or buckles unexpectedly, ligament damage likely rules out partial replacement.
- Have conservative treatments (physiotherapy, injections, pain relief) failed to provide lasting relief?
Surgery is considered only after non-surgical options have been exhausted. If you have not yet tried structured physiotherapy or corticosteroid injections, your consultant will likely recommend these first.
- Are you able to achieve near-full knee extension and flexion despite pain?
Severe stiffness or fixed flexion deformity complicates partial replacement. A reasonable range of motion is typically required for successful implantation and post-operative function.
This self-assessment provides provisional guidance only. Definitive candidacy determination requires clinical examination, weight-bearing X-rays, and specialist consultation. Do not self-diagnose suitability.
One final nuance often overlooked: patellofemoral osteoarthritis—arthritis affecting the kneecap joint—is no longer considered an absolute contraindication to partial replacement, provided you have been counselled on the uncertainty of outcomes. This NHS commissioning policy sets out that the procedure must be undertaken by a surgeon who can evidence a minimum of 12 unicompartmental knee replacements per year, with audit data submitted annually. Surgeon volume is not vanity—it is a validated proxy for technical proficiency and implant positioning accuracy, both of which directly influence how long your new joint lasts.
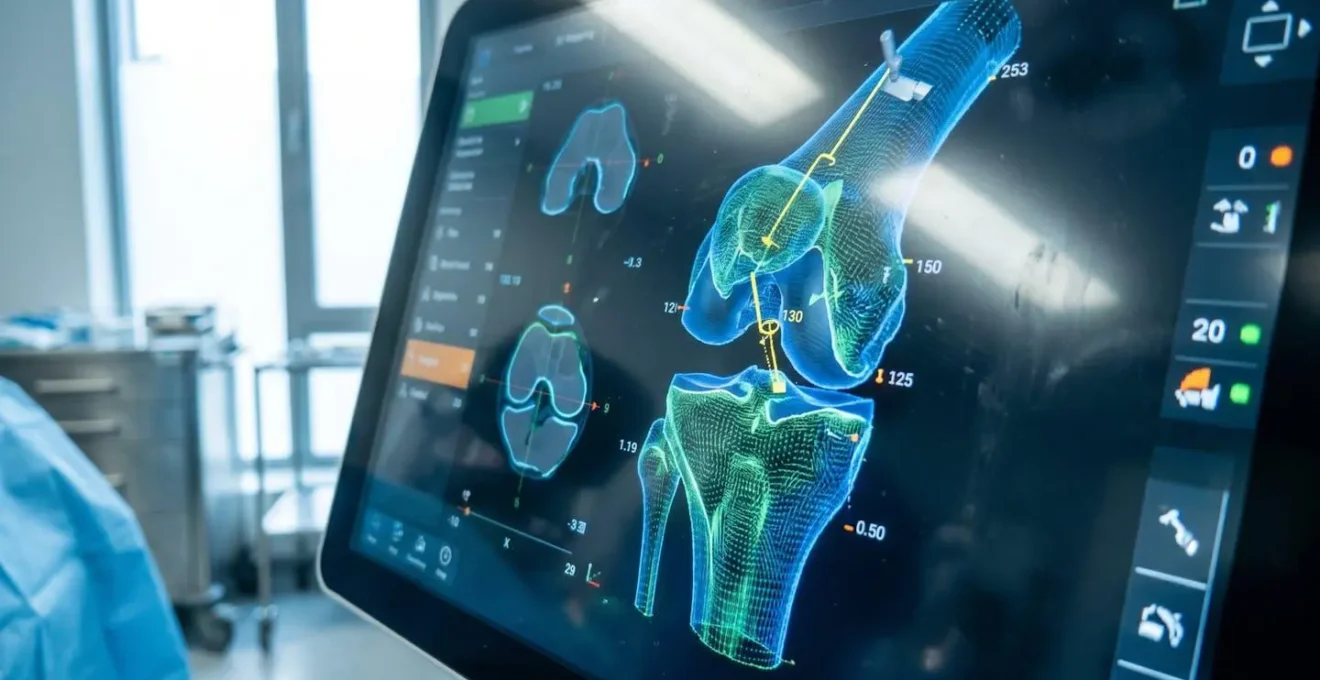
Robotic Precision: How the Procedure Works
For patients whose clinical assessment confirms candidacy, the next decision involves surgical technique. Consulting an experienced knee replacement surgeon who specializes in robotic-assisted techniques is essential to evaluate whether this technological approach offers measurable advantages over traditional manual instrumentation. Robotic-assisted partial knee replacement operates through a symbiosis of pre-operative planning and intra-operative execution. Before you enter the operating theatre, CT or MRI scans create a three-dimensional digital model of your unique knee anatomy. The surgeon uses this virtual blueprint to plan the precise size, position, and alignment of the implant components—work that happens days before the first incision.
On the day of surgery, the robotic arm functions not as an autonomous entity, but as an extension of the surgeon’s expertise. Once the knee is exposed through a smaller incision (typically 8-10 centimetres, compared to 15-20 centimetres for total replacement), the surgeon registers anatomical landmarks that calibrate the robotic system to your actual joint. The robotic arm then guides bone preparation with sub-millimetre accuracy, constraining the cutting tools to the pre-planned boundaries. If the surgeon attempts to deviate from the optimal alignment—even by fractions of a degree—the system provides haptic resistance, preventing imprecise bone resection. This technological guardrail is where robotic systems deliver their primary advantage: enhanced implant positioning accuracy.
Robotic Precision: The Technical Advantage
Computer-guided pre-operative planning maps your individual knee anatomy in three dimensions, allowing the surgeon to simulate implant positioning before surgery begins. During the procedure, real-time intra-operative adjustment ensures the implant sits within the planned alignment corridor. Comparative studies suggest robotic assistance improves implant alignment precision by approximately 30-40% relative to traditional manual techniques, reducing the risk of early implant loosening caused by sub-optimal positioning. The technology does not replace surgical judgement—it amplifies it, enabling reproducible accuracy across varying patient anatomies.
The implant comprises two components: a metal femoral component that replaces the worn cartilage surface on the thighbone, and a polyethylene tibial component that resurfaces the shinbone plateau. Unlike total replacement, which removes all three knee compartments, partial replacement leaves the healthy lateral compartment, cruciate ligaments, and kneecap articulation untouched. This preservation explains why patients report the knee “feels more natural”—because the majority of your original knee remains.
Surgical duration averages 60-90 minutes under general or spinal anaesthesia. Most patients are mobilized the same afternoon or following morning. Hospital stay typically spans 1-2 nights, markedly shorter than the 3-5 nights often required after total knee replacement.

Your Recovery Journey: Timeline and Milestones
Recovery from partial knee replacement follows a predictable arc, though individual variation exists based on age, baseline fitness, and adherence to physiotherapy. The first fortnight centres on wound healing, gentle range-of-motion exercises, and transitioning from crutches to a walking stick. Pain during this phase is typically well-controlled with oral analgesics, and most patients describe discomfort as significantly less intense than the pre-operative arthritis pain they endured for months or years.
-
Hospital discharge (day 1-2), gentle mobilization with physiotherapy guidance, use of crutches for protected weight-bearing, wound inspection, and ice application to manage swelling. Knee flexion typically reaches 90 degrees by end of week two.
-
Progressive weight-bearing as tolerated, transition from crutches to single walking stick, formal physiotherapy sessions focusing on quadriceps strengthening, hamstring flexibility, and proprioceptive balance exercises. Most patients achieve independent walking without aids by week 4-5.
-
Strength building through resistance exercises, restoration of full range of motion (target: 0-130 degrees flexion), gradual return to low-impact activities such as swimming, cycling, and brisk walking. Driving typically resumes at 4-6 weeks if right knee, once emergency stop can be performed safely. Return to golf, doubles tennis, or hiking usually occurs by month 4-6.
-
Full functional recovery with completion of supervised physiotherapy program. Patients transition to independent maintenance exercise routines. Kneeling tolerance varies—some regain the ability to kneel comfortably, whilst others experience mild discomfort over the implant site that diminishes over 12-18 months.
Physiotherapy plays a pivotal role throughout this trajectory. Structured rehabilitation protocols focus on three pillars: restoring joint flexibility, rebuilding quadriceps and hamstring strength, and re-establishing proprioceptive balance to prevent falls. The preserved cruciate ligaments in your partially replaced knee maintain natural sensory feedback, making balance re-education faster and more intuitive compared to total replacement, where ligaments are often sacrificed.
Adherence to this rehabilitation trajectory requires active patient participation—passive recovery is insufficient. The following priorities determine whether you achieve optimal functional outcomes or settle for suboptimal range of motion and persistent weakness that could have been prevented through structured effort.
- Attend physiotherapy sessions and perform daily home exercises to optimize outcomes
- Avoid high-impact activities until consultant clearance, typically 6-9 months post-surgery
- Monitor for warning signs: persistent fever, wound inflammation, severe pain, or calf swelling
- Maintain ideal body weight to reduce implant stress and preserve longevity
Returning to work depends on occupation. Sedentary roles (desk-based office work) typically permit return within 4-6 weeks. Physically demanding jobs requiring prolonged standing, kneeling, or lifting may necessitate 8-12 weeks off or modified duties during the transition period. Discuss realistic return-to-work timelines with your surgeon and occupational health team before surgery to arrange appropriate sick leave.
Durability and Long-Term Outcomes: What the Data Shows
The question patients ask most frequently after candidacy is confirmed: “How long will it last?” Les données 2025 du National Joint Registry confirment que over 4.5 million joint replacement procedures have been recorded since April 2003, with the 22nd Annual Report documenting a continued year-on-year reduction in revision surgery rates. This trend provides robust evidence that implants are lasting longer and that patient outcomes have improved as surgical techniques, implant designs, and patient selection protocols have been refined.
10-20years
Typical implant lifespan in appropriately selected patients, with some lasting beyond two decades
Registry analyses consistently show that implant survival at 10 years exceeds 90% when strict patient selection criteria are applied. The critical determinant is not the implant itself—modern materials demonstrate excellent wear characteristics—but whether your arthritis remains confined to the replaced compartment. If osteoarthritis progresses into the untreated lateral or patellofemoral compartments over subsequent years, revision to total knee replacement becomes necessary. This progression occurs in approximately 10-15% of patients within the first decade according to long-term registry follow-up studies, most commonly in those who were borderline candidates at the time of initial surgery.
Patient-reported outcome measures reveal high satisfaction rates. The majority of individuals describe significant improvements in pain relief, functional mobility, and quality of life. The ability to kneel, squat, and engage in recreational activities often surpasses what total replacement permits, precisely because natural knee anatomy is largely preserved. Younger, more active patients frequently report that the knee “feels like their own joint” rather than an artificial construct—a qualitative outcome that registry data struggles to capture but that patients value enormously.
Factors influencing longevity include patient age at surgery (younger patients place higher cumulative demands on the implant), body weight (obesity accelerates polyethylene wear), activity level (high-impact sports increase stress), and underlying disease progression. Maintaining a healthy weight, adhering to activity modification guidelines, and attending annual follow-up appointments allow early detection of implant loosening or arthritis progression before catastrophic failure occurs.
How long before I can walk my dog again after partial knee replacement?
Short, gentle walks on level ground typically resume within 2-3 weeks post-surgery using a walking stick for balance. Longer walks (30-60 minutes) and uneven terrain usually become comfortable by 6-8 weeks, once quadriceps strength has been partially restored through physiotherapy. Vigorous off-lead activities where your dog might pull suddenly should wait until 3-4 months when joint stability and proprioception have fully recovered.
Will the implant set off airport security scanners?
Modern knee implants contain sufficient metal to occasionally trigger airport metal detectors. Carry your surgical discharge summary or implant identification card when travelling. Security staff are familiar with joint replacements and will typically perform a secondary hand-held scan or pat-down if the alarm activates.
Can I kneel comfortably after the operation, or will gardening remain difficult?
Kneeling tolerance varies significantly between patients. Some regain comfortable kneeling by 6-9 months post-surgery, whilst others experience persistent discomfort over the implant site that improves but never fully resolves. Using knee pads or kneeling cushions often makes gardening feasible. Your surgeon cannot guarantee full kneeling comfort, so discuss realistic expectations during your pre-operative consultation if kneeling is essential to your hobbies or occupation.
What happens if my arthritis spreads to other parts of my knee in the future?
If osteoarthritis progresses into the untreated compartments—which occurs in 10-15% of patients within 10 years—revision surgery to convert the partial replacement into a total knee replacement becomes necessary. This revision is more complex than a primary total replacement but remains a well-established procedure. Annual follow-up X-rays help detect early arthritis progression before symptoms become severe.
Is robotic-assisted surgery safer or more effective than traditional manual techniques?
Robotic assistance enhances implant positioning precision, potentially reducing the risk of alignment-related complications such as early loosening. However, surgeon experience and patient selection remain the dominant factors determining outcomes. When available, robotic technology offers measurable advantages in reproducible accuracy, but it complements—rather than replaces—surgical expertise.
How do I know if my surgeon is qualified and performs enough procedures to maintain expertise?
NHS commissioning policies mandate that surgeons performing unicompartmental knee replacements must complete a minimum of 12 procedures annually and submit audit data to demonstrate outcomes. When consulting a surgeon, ask directly about their annual case volume, revision rates, and whether they participate in the National Joint Registry. Do not hesitate to request evidence of their credentials, training in robotic-assisted techniques (if applicable), and membership with the British Orthopaedic Association.
For those seeking to understand the broader landscape of contemporary surgical options and technological advances, exploring this overview of modern knee surgery provides comprehensive context for understanding where partial replacement fits within the full spectrum of treatment approaches available in 2026. Surgical innovation continues to refine techniques, implant materials, and patient selection algorithms, steadily improving the durability and functional outcomes that define successful joint replacement.
- Request GP referral to orthopedic consultant with annual case volume exceeding 12 procedures
- Obtain copies of recent knee X-rays and MRI scans for initial consultation
- Prepare written questions about surgical technique, recovery milestones, and surgeon’s revision rates
- Verify surgeon participates in National Joint Registry and review their outcome data
Partial knee replacement represents a targeted intervention for a specific subset of patients—those whose arthritis remains localized, whose ligaments remain functional, and whose expectations align with the procedure’s capabilities. When these conditions converge, the surgery delivers exceptional pain relief, rapid recovery, and durability that can span two decades or more. The critical variable is not the implant, the technology, or even the surgeon’s skill in isolation—it is the disciplined application of evidence-based patient selection criteria that registry data has validated over 4.5 million procedures and 22 years of continuous monitoring.
Limitations of this guide:
- This guide provides general educational information and cannot replace personalized assessment by an orthopedic specialist
- Candidacy criteria, surgical techniques, and recovery protocols vary based on individual patient anatomy, age, activity level, and overall health
- Success rates, implant longevity, and complication risks mentioned are population averages and may not reflect individual outcomes
Risks to be aware of:
- Risk of implant failure requiring revision surgery if arthritis progresses to other knee compartments
- Risk of infection, blood clots, or implant loosening (occurs in fewer than 5% of cases within 10 years)
- Risk of incomplete pain relief if patient selection criteria are not strictly met
Essential next step: Consult a qualified orthopedic surgeon specializing in knee arthroplasty for clinical examination, imaging assessment, and discussion of whether partial knee replacement is appropriate for your specific condition and lifestyle requirements.